Introduction
The skin is the most superficial part of the body. The signs of ageing are most visible in the skin. Although, ageing skin is not a threat to a person, it can have a detrimental effect on the psychology of a person. A look into the causes of skin ageing, the available treatments and preventive measures for this inevitable change is important to help both the already aged, as well as, the youth.
This is a 4 part article in which:
- Part 1 – Discusses the structure of skin and its different components (current article)
- Part 2 – Discusses cutaneous ageing and its causes
- Part 3 – Discusses the characteristics of ageing skin and the changes in skin appearance
- Part 4 – Discusses products and treatments for skin ageing
a) Sunscreen Agents
b) Moisturizers
c) Antioxidants
d) Make Up
e) Dermal Fillers
f) Chemical Peels
g) Botulinum Toxin
h) Estrogen and Hormonal Treatments
i) Plastic Surgery
Part 1 – Introduction and Structure of Skin
What Is Ageing?
Ageing is the process of growing old. It is a continuous time dependent and multifactorial phenomenon of reduction in size and number of cells and also reduction in the rate of many organic functions both at cellular and molecular levels. Skin is the largest and the most superficial organ of the body which is exposed to infection, disease and injury. It also shows the signs of ageing the earliest. Skin functions that have shown to decline are cell replacement, injury response, barrier function, sensory perception, immune and vascular responsiveness, thermoregulation, sweat production, sebum production and vitamin D production.1
The Skin
Skin is the largest organ of the body in terms of surface area and weight. It covers all the external surface of the body. It protects the body, helps maintain a constant body temperature and provides sensory information about the surrounding environment. Of all the bodies organs skin is most exposed to infection, disease and injury.2,3
Structure Of The Skin2.3,11
Skin consists of 2 main parts the superficial, thinner portion is the epidermis and the deeper thicker part is the dermis. Deep to dermis is the subcutaneous layer which is not a part of the skin. The subcutaneous layer serves as a storage depot for fat and contains large blood vessels which supply the skin with nutrients. It also contains nerve endings called Pacinian corpuscles that are sensitive to pressure.
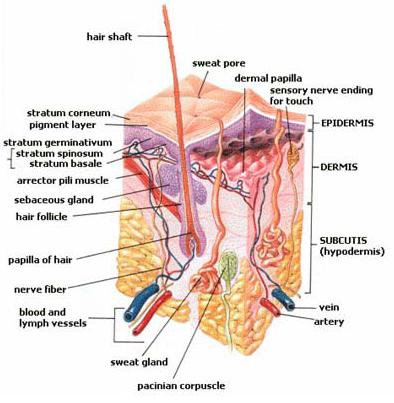
Epidermis2.3,11
It consists of 4 principle cells
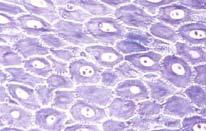
i) Keratinocytes – They make up 90% of the epidermis layer of the skin and they produce the protein keratin. The protein protects the skin and underlying tissues from heat, microbes and chemicals. It also produces lamellar granules which release a water repellent sealant.
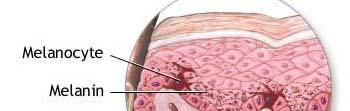
ii) Melanocytes – They make up 8% of the epidermis. It produces a pigment melanin which contributes to the colour of the skin and absorbs damaging ultraviolet light.
iii) Langerhans Cells – They arise from red bone marrow and migrate to the epidermis. They participate in immune response against microbes that invade the skin and these cells are easily damaged by ultraviolet light.
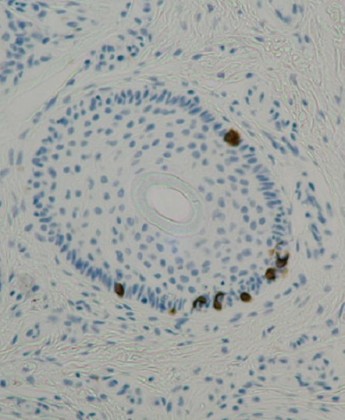
iv) Merkel Cells – They are usually located in the deepest layer of the epidermis. These cells are in contact with the flattened process of a sensory neuron structure called tactile disc. Merkel cells and tactile disc together detect different aspects of touch sensation.
LAYERS OF EPIDERMIS
Epidermis of the skin usually has 4 layers but few areas where exposure to friction is greatest e.g. fingertips, palms, soles, etc. have 5 layers. The layers are:‐
i) Stratum Basale – It is the deepest layer of epidermis and has a single layer of keratinocytes. It is also known as stratum germinativum.
ii) Stratum Spinosum – It is superficial to the stratum basale. It provides both strength and flexibility to the skin. This layer consists of 8‐10 layers of keratinocytes.
iii) Stratum Granulosum – It is middle layer of the epidermis. It consists of protein called keratohyalin which converts tonofilaments into keratin. This layer consists of 3‐5 layers of flattened keratinocytes. Also present in the Keratinocytes are membrane enclosed lamellar granules which release lipid rich secretion. This secretion fills the space between cells of stratum granulosum, stratum lucidum and stratum corneum. They act as a water repellent sealant that helps retard loss of body fluids and entry of foreign materials.
iv) Stratum Lucidum – This layer is present only in those areas which are prone to friction i.e. in thick skin. It consists of large amount of keratin and thickened plasma membrane. The layer is made up of 3‐5 layers of flattened dead keratinocytes.
V) Stratum Corneum – This layer consists of 25‐30 layers of flattened dead keratinocytes. These are continuously shed and replaced by cells from the deeper strata. This layer consists of mostly keratin and lipid secretions from lamellar granules which make this layer an effective water repellent barrier. Multiple layers of dead cells protect the deeper layers from injury and microbial invasion.
Dermis2.3,11
Dermis is composed mainly of connective tissues containing collagen and elastic fibers. Cells present in dermis include:‐
i) Fibroblast – They provide the structural framework for many tissues and play a critical role in wound healing. They are also responsible for synthesizing the dermal proteins.
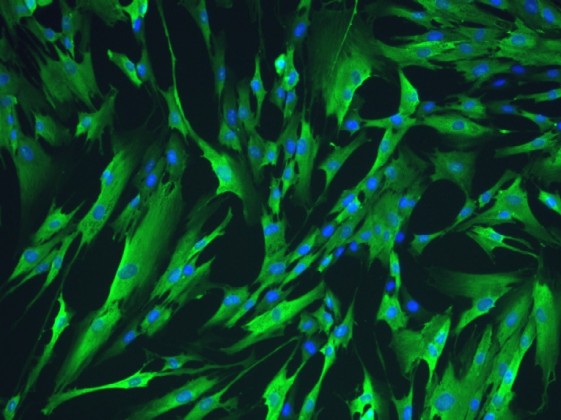
ii) Macrophages – They are also called as big eaters as their role is to phagocytose cellular debris and pathogens.
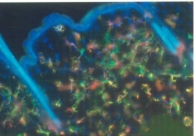
iii) Adipocytes – They are cells specialized in storing energy as fat.
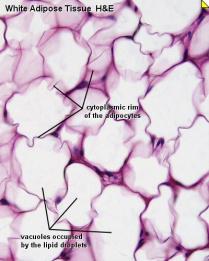
Based upon the tissue structure dermis is divided into 2 regions
i) Papillary region – It is a superficial part of the dermis. The surface area of the papillary region is greatly increased by small fingerlike projection called dermal papillae. Some dermal papillae contain tactile receptors called corpuscles of touch or Meissner corpuscles these are nerve endings that are sensitive to touch. Also present in dermal papillae are free nerve endings which initiate signal which gives rise to sensation of warmth, coolness, pain, tickling and itching.
ii) Reticular region – It is the deeper part of dermis. In this region bundles of collagen fibers are interlaced in a net like manner. Adipose cells, hair follicles, nerves, sebaceous glands, sweat glands occupy the space between the fibers. Combination of collagen and elastic fibers in reticular region is responsible for providing the skin with strength, extensibility and elasticity.
DERMAL MATRIX COMPONENTS
I] COLLAGEN‐ is a primary structural component of the dermis and the most abundant protein found in humans. It is responsible for conferring the strength and support to human skin.
II] ELASTIN‐ it is a protein in the connective tissue that is elastic and allows many tissues in the body to resume their shape after stretching or contraction. It helps the skin to return to its original position when it is pinched or poked.
III] GLYCOSAMINOGLYCANS‐ It is a constituent of the dermal skin along with collagen and elastin and is responsible for conferring the outward appearance of the skin. They are composed of polysaccharides, with repeating disaccharide units attached to a core protein. They exhibit the capacity to bind water up to 1000 times their volume. The most important of the glycosaminoglycan family is hyaluronic acid. Others include dermatan sulphate, chondroitin sulphate. They render normal skin plump, soft and hydrated and maintain proper water and salt balance. Hyaluronic acid is found at the periphery of collagen and elastin fibers and where these fibers intersect. It is found in all connective tissues and is produced by fibroblast and keratinocytes in the skin. Hyaluronic acid is localized not only in the dermis but also in the epidermal intercellular spaces.
References
- Elderly skin and its rejuvenation: products and procedures for the aging skin, Marcia Ramos‐e‐Silva et. al., Journal of Cosmetic Dermatology, 6, 40–50.
- Principles of Anatomy and Physiology, Gerard J Tortora, John Wiley & Sons Inc. Chapter 5– The Integumentary System (pg 139 – 145)
- http://en.wikipedia.org/wiki/Skin (accessed on March 03, 2011)
- http://www.web-books.com/eLibrary/Medicine/Physiology/Skin/Skin.htm (accessed on March 03, 2011)
- http://byhealth.com/skin-integumentary-system (accessed on March 03, 2011)
- http://pathology.class.kmu.edu.tw/ch10/Slide104.htm (accessed on March 03, 2011)
- Solitary Merkel cells in the normal skin, expressing cytokeratin-20. Koljonen World Journal of Surgical Oncology 2006 4:7.
- http://www.nctimes.com/app/blogs/wp/?p=10723 (accessed on March 03, 2011)
- Marcel Dupasquier et. al. Macrophages and Dendritic Cells Constitute a Major Subpopulation of Cells in the Mouse Dermis. Journal of Investigative Dermatology (2004) 123, 876–879.
- http://www.lab.anhb.uwa.edu.au/mb140/corepages/connective/connect.htm (accessed on March 03, 2011)
- McGrath, J.A.; Eady, R.A.; Pope, F.M. (2004). Rook’s Textbook of Dermatology (7th ed.). Blackwell Publishing. pp. 3.1–3.6

![Figure 6 - Layers of epidermis: [B] = Stratum Basale, [S] = Stratum Spinosum, [G] = Stratum Granulosum, [C] Stratum Corneum Figure 6 - Layers of epidermis: [B] = Stratum Basale, [S] = Stratum Spinosum, [G] = Stratum Granulosum, [C] Stratum Corneum](https://pharmaxchange.info/wp-content/uploads/2011/03/Figure-6-Layers-of-epidermis.jpg)
Pingback: What Causes Blisters
Pingback: Answer My Health Question » The Structure of Skin
Pingback: skin | kimsojung