Niosomes are a novel drug delivery system, in which the medication is encapsulated in a vesicle. The vesicle is composed of a bilayer of non-ionic surface active agents and hence the name niosomes. The niosomes are very small, and microscopic in size. Their size lies in the nanometric scale. Although structurally similar to liposomes, they offer several advantages over them. Niosomes have recently been shown to greatly increase transdermal drug delivery and also can be used in targeted drug delivery, and thus increased study in these structures can provide new methods for drug delivery.
Structure of Niosomes:
Niosomes are microscopic lamellar structures, which are formed on the admixture of non-ionic surfactant of the alkyl or dialkyl polyglycerol ether class and cholesterol with subsequent hydration in aqueous media1.
Structurally, niosomes are similar to liposomes, in that they are also made up of a bilayer. However, the bilayer in the case of niosomes is made up of non-ionic surface active agents rather than phospholipids as seen in the case of liposomes. Most surface active agents when immersed in water yield micellar structures, however some surfactants can yield bilayer vesicles which are niosomes.
Niosomes may be unilamellar or multilamellar depending on the method used to prepare them.
The niosome is made of a surfactant bilayer with its hydrophilic ends exposed on the outside and inside of the vesicle, while the hydrophobic chains face each other within the bilayer. Hence, the vesicle holds hydrophilic drugs within the space enclosed in the vesicle, while hydrophobic drugs are embedded within the bilayer itself. The figure below will give a better idea of what a niosome looks like and where the drug is located within the vesicle.
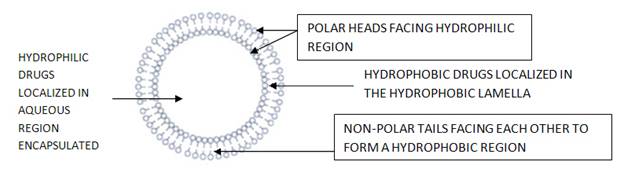
A typical niosome vesicle would consist of a vesicle forming ampiphile i.e. a non-ionic surfactant such as Span-60, which is usually stabilized by the addition of cholesterol and a small amount of anionic surfactant such as diacetyl phosphate, which also helps in stabilizing the vesicle2.
Method of Preparation of Niosomes
Niosomes can be prepared by a number of methods which are as follows:
- Ether injection method: In this method, a solution of the surfactant is made by dissolving it in diethyl ether. This solution is then introduced using an injection (14 gauge needle) into warm water or aqueous media containing the drug maintained at 60°C. Vaporization of the ether leads to the formation of single layered vesicles. The particle size of the niosomes formed depend on the conditions used, and can range anywhere between 50-1000µm3.
- Hand shaking method (Thin Film Hydration Technique): In this method a mixture of the vesicle forming agents such as the surfactant and cholesterol are dissolved in a volatile organic solvent such as diethyl ether or chloroform in a round bottom flask. The organic solvent is removed at room temperature using a rotary evaporator, which leaves a thin film of solid mixture deposited on the walls of the flask. This dried surfactant film can then be rehydrated with the aqueous phase, with gentle agitation to yield multilamellar niosomes. The multilamellar vesicles thus formed can further be processed to yield unilamellar niosomes or smaller niosomes using sonication, microfluidization or membrane extrusion techniques3.
- Reverse phase evaporation technique: This method involves the creation of a solution of cholesterol and surfactant (1:1 ratio) in a mixture of ether and chloroform. An aqueous phase containing the drug to be loaded is added to this, and the resulting two phases are sonicated at 4-5°C. A clear gel is formed which is further sonicated after the addition of phosphate buffered saline (PBS). After this the temperature is raised to 40°C and pressure is reduced to remove the organic phase. This results in a viscous niosome suspension which can be diluted with PBS and heated on a water bath at 60°C for 10 mins to yield niosomes4.
- Trans membrane pH gradient (inside acidic) Drug Uptake Process (remote loading): In this method, a solution of surfactant and cholesterol is made in chloroform. The solvent is then evaporated under reduced pressure to get a thin film on the wall of the round bottom flask, similar to the hand shaking method. This film is then hydrated using citric acid solution (300mM, pH 4.0) by vortex mixing. The resulting multilamellar vesicles are then treated to three freeze thaw cycles and sonicated. To the niosomal suspension, aqueous solution containing 10mg/ml of drug is added and vortexed. The pH of the sample is then raised to 7.0-7.2 using 1M disodium phosphate (this causes the drug which is outside the vesicle to become non-ionic and can then cross the niosomal membrane, and once inside it is again ionized thus not allowing it to exit the vesicle). The mixture is later heated at 60°C for 10 minutes to give niosomes5.
- The “Bubble” Method: It is a technique which has only recently been developed and which allows the preparation of niosomes without the use of organic solvents. The bubbling unit consists of a round bottom flask with three necks, and this is positioned in a water bath to control the temperature. Water-cooled reflux and thermometer is positioned in the first and second neck, while the third neck is used to supply nitrogen. Cholesterol and surfactant are dispersed together in a buffer (pH 7.4) at 70°C. This dispersion is mixed for a period of 15 seconds with high shear homogenizer and immediately afterwards, it is bubbled at 70°C using the nitrogen gas to yield niosomes6.
- Formation of Proniosomes and Niosomes from Proniosomes: To create proniosomes, a water soluble carrier such as sorbitol is first coated with the surfactant. The coating is done by preparing a solution of the surfactant with cholesterol in a volatile organic solvent, which is sprayed onto the powder of sorbitol kept in a rotary evaporator. The evaporation of the organic solvent yields a thin coat on the sorbitol particles. The resulting coating is a dry formulation in which a water soluble particle is coated with a thin film of dry surfactant. This preparation is termed Proniosome7.
The niosomes can be prepared from the proniosomes by adding the aqueous phase with the drug to the proniosomes with brief agitation at a temperature greater than the mean transition phase temperature of the surfactant.
Advantages of Niosomes
Use of niosomes in cosmetics was first done by L’Oreal as they offered the following advantages2:
- The vesicle suspension being water based offers greater patient compliance over oil based systems
- Since the structure of the niosome offers place to accommodate hydrophilic, lipophilic as well as ampiphilic drug moieties, they can be used for a variety of drugs.
- The characteristics such as size, lamellarity etc. of the vesicle can be varied depending on the requirement.
- The vesicles can act as a depot to release the drug slowly and offer a controlled release.
Other advantages of niosomes are:
- They are osmotically active and stable.
- They increase the stability of the entrapped drug
- Handling and storage of surfactants do not require any special conditions
- Can increase the oral bioavailability of drugs
- Can enhance the skin penetration of drugs
- They can be used for oral, parenteral as well topical use
- The surfactants are biodegradable, biocompatible, and non-immunogenic
- Improve the therapeutic performance of the drug by protecting it from the biological environment and restricting effects to target cells, thereby reducing the clearance of the drug.
- The niosomal dispersions in an aqueous phase can be emulsified in a non-aqueous phase to control the release rate of the drug and administer normal vesicles in external non-aqueous phase.
Comparison of Niosome v/s Liposome
Niosomes are different from liposomes in that they offer certain advantages over liposomes. Liposomes face problems such as –they are expensive, their ingredients like phospholipids are chemically unstable because of their predisposition to oxidative degradation, they require special storage and handling and purity of natural phospholipids is variable. Niosomes do not have any of these problems. Also since niosomes are made of uncharged single-chain surfactant molecules as compared to the liposomes which are made from neutral or charged double chained phospholipids, the structure of niosomes is different from that of liposomes.
However Niosomes are similar to liposomes in functionality. Niosomes also increase the bioavailability of the drug and reduce the clearance like liposomes. Niosomes can also be used for targeted drug delivery, similar to liposomes. As with liposomes, the properties of the niosomes depend both- on the composition of the bilayer, and the method of production used.
Applications of Niosomes
The application of niosomal technology is widely varied and can be used to treat a number of diseases. The following are a few uses of niosomes which are either proven or under research.
- Drug Targetting:
One of the most useful aspects of niosomes is their ability to target drugs. Niosomes can be used to target drugs to the reticulo-endothelial system. The reticulo-endothelial system (RES) preferentially takes up niosome vesicles. The uptake of niosomes is controlled by circulating serum factors called opsonins. These opsonins mark the niosome for clearance. Such localization of drugs is utilized to treat tumors in animals known to metastasize to the liver and spleen. This localization of drugs can also be used for treating parasitic infections of the liver1.
Niosomes can also be utilized for targeting drugs to organs other than the RES. A carrier system (such as antibodies) can be attached to niosomes (as immunoglobulins bind readily to the lipid surface of the niosome) to target them to specific organs. Many cells also possess the intrinsic ability recognize and bind specific carbohydrate determinants, and this can be exploited by niosomes to direct carrier system to particular cells8.
- Anti-neoplastic Treatment:
Most antineoplastic drugs cause severe side effects. Niosomes can alter the metabolism, prolong circulation and half life of the drug, thus decreasing the side effects of the drugs. Niosomal entrapment of Doxorubicin and Methotrexate (in two separate studies) showed beneficial effects over the unentrapped drugs, such as decreased rate of proliferation of the tumor and higher plasma levels accompanied by slower elimination9.
- Leishmaniasis:
Leishmaniasis is a disease in which a parasite of the genus Leishmania invades the cells of the liver and spleen. Commonly prescribed drugs for the treatment are derivatives of antimony (antimonials), which in higher concentrations can cause cardiac, liver and kidney damage. Use of niosomes in tests conducted showed that it was possible to administer higher levels of the drug without the triggering of the side effects, and thus allowed greater efficacy in treatment10.
- Delivery of Peptide Drugs:
Oral peptide drug delivery has long been faced with a challenge of bypassing the enzymes which would breakdown the peptide. Use of niosomes to successfully protect the peptides from gastrointestinal peptide breakdown is being investigated. In an invitro study conducted by Yoshida et al, oral delivery of a vasopressin derivative entrapped in niosomes showed that entrapment of the drug significantly increased the stability of the peptide11.
- Use in Studying Immune Response:
Due to their immunological selectivity, low toxicity and greater stability; niosomes are being used to study the nature of the immune response provoked by antigens12.
- Niosomes as Carriers for Haemoglobin:
Niosomes can be used as carriers for haemoglobin within the blood. The niosomal vesicle is permeable to oxygen and hence can act as a carrier for haemoglobin in anemic patients13.
- Transdermal Drug Delivery Systems Utilizing Niosomes:
One of the most useful aspects of niosomes is that they greatly enhance the uptake of drugs through the skin. Transdermal drug delivery utilizing niosomal technology is widely used in cosmetics, in fact, it was one of the first uses of the niosomes. Topical use of niosome entrapped antibiotics to treat acne is done. The penetration of the drugs through the skin is greatly increased as compared to un-entrapped drug14.
Recently, transdermal vaccines utilizing niosomal technology is also being researched. A study conducted by P. N. Gupta et al has shown that niosomes (along with liposomes and transfersomes) can be utilized for topical immunization using tetanus toxoid. However, the current technology in niosomes allows only a weak immune response, and thus more research needs to be done in this field.
- Other Applications:
Niosomes can also be utilized for sustained drug release and localized drug action to greatly increase the safety and efficacy of many drugs. Toxic drugs which need higher doses can possibly be delivered safely using niosomal encapsulation15.
Marketed Products
Lancome has come out with a variety of anti-ageing products which are based on niosome formulations. L’Oreal is also conducting research on anti-ageing cosmetic products.
Books on Niosomes
Check out some useful books on niosomes
Conclusion
Over the years, there has been a great evolution in drug delivery technologies. Niosomal drug delivery systems are an example of one of the various drug delivery systems available. The technology utilized in niosomes is still greatly in its infancy, and already it is showing promise in the fields of cancer and infectious disease treatments. The system is already in use for various cosmetic products. Niosomes represent a promising drug delivery technology and much research has to be inspired in this to juice out all the potential in this novel drug delivery system.
References
- Malhotra M. and Jain N.K. Niosomes as Drug Carriers. Indian Drugs (1994), 31 (3): 81-86.
- Buckton G., Harwood, Interfacial phenomena in Drug Delivery and Targeting Academic Publishers, Switzerland. 1995; p.154-155.
- Baillie A.J., Coombs G.H. and Dolan T.F. Non-ionic surfactant vesicles, niosomes, as delivery system for the anti-leishmanial drug, sodium stribogluconate J.Pharm.Pharmacol. 1986; 38: 502-505.
- Raja Naresh R.A., Chandrashekhar G., Pillai G.K. and Udupa N. Antiinflammatory activity of Niosome encapsulated diclofenac sodium with Tween -85 in Arthitic rats. Ind.J.Pharmacol. 1994; 26:46-48.
- Maver L.D. Bally M.B. Hope. M.J. Cullis P.R. Biochem Biophys. Acta (1985), 816:294-302.
- Chauhan S. and Luorence M.J. The preparation of polyoxyethylene containing non-ionic surfactant. vesicles. J. Pharm. Pharmacol. 1989; 41: 6p.
- Blazek-Walsh A.I. and Rhodes D.G. Pharm. Res. SEM imaging predicts quality of niosomes from maltodextrin-based proniosomes. 2001; 18: 656-661.
- Gregoriadis G. Targeting of drugs: implications in medicine. Lancet. 1981; 2(8240): 241-246.
- Cummings J., Staurt J.F. and Calman K.C. Determination of adriamycin, adriamycinol and their 7-deoxyaglycones in human serum by high-performance liquid chromatography. J. Chromatogr. 1984; 311: 125-133.
- Hunter C.A., Dolan T.F., Coombs G.H. and Baillie A.J. Vesicular systems (niosomes and liposomes) for delivery of sodium stibogluconate in experimental murine visceral leishmaniasis. J.Pharm. Pharmacol. 1988; 40(3): 161-165.
- Yoshioka T., Sternberg B., Moody M. and Florence A.T. Niosomes from Span surfactants: Relations between structure and form. J. Pharm. Pharmcol. Supp. 1992; 44: 1044.
- Brewer J.M. and Alexander J.A. The adjuvant activity of non-ionic surfactant vesicles (niosomes) on the BALB/c humoral response to bovine serum albumin. Immunology. 1992; 75 (4) :570-575.
- Moser P., Marchand-Arvier M., Labrude P., Handjani Vila. R.M. and Vignerson C. Niosomes d’hémoglobine. I. Preparation, proprietes physicochimiques et oxyphoriques, stabilite. Pharma. Acta.Helv. 1989; 64 (7): 192-202.
- Jayaraman C.S., Ramachandran C. and Weiner N. Topical delivery of erythromycin from various formulations: an in vivo hairless mouse study. J. Pharm. Sci. 1996; 85 (10): 1082-1084.
- Azmin M.N., Florence A.T., Handjani-Vila R.M., Stuart J.F.B., Vanlerberghe G., and Whittaker J.S. The effect of non-ionic surfactant vesicle (niosome) entrapment on the absorption and distribution of methotrexate in mice. J. Pharm. Pharmacol. 1985;37: 237–242.

thank u
very nice
good one